WHAT CAUSES PILES?
Piles may be caused due to a variety of reasons and it may not be possible to point out the exact cause in every individual. However, the commonest causes are as follows:
- Long standing constipation
- Excessive straining during bowel movements over a long period of time, or very hard stools that are not excreted smoothly
- Family history of piles
- Faulty toilet habits – for example, some people have a habit of spending too much time in the toilet, straining while they read, work on cell phones etc.
- Pregnancy and childbirth – An increase in the hormone Progesterone causes the blood vessels to relax which leads to pooling of blood in them. Also, the pressure of the growing uterus on the vessels prevents them from emptying completely
- An unhealthy lifestyle – Lack of exercise, stress, alcohol, smoking
- Obesity – Piles is more common in the overweight
- Lifting heavy weights
WHAT ARE THE SYMPTOMS OF PILES?
Hemorrhoids may remain silent and not cause any symptoms! Contrary to popular belief, they are usually painless. When evident, some of the common symptoms include:
- Bleeding during a bowel movement. Most of the times this is painless. There may be fresh blood at the end of passing stools or you may witness blood on the tissue.
- You may feel a lump outside the anus. In the earlier stages, this swelling may be felt only on straining and may go back once the pressure is released. As the disease progresses, the lump is permanently on the outside and is constantly felt.
- Piles may cause itching in the region aka Perianal pruritus.
- There may be discharge, causing soiling of undergarments.
- There may be a sensation of stool being ‘stuck’ at the anal region after a bowel movement.
- Rarely, there may be dull pain.
- As a complication, the hemorrhoid sometimes develops a clot ( Thrombosed Hemorrhoid ). This may cause the development of sudden pain which worsens on sitting or during movement.
HOW ARE PILES DIAGNOSED?
With almost one in every two adults being affected by piles at some stage of their life, there is no need for one to be embarrassed or frightful of piles. In fact, the earlier you seek help, the better the chances that you will be free of piles with minimal treatment.
After obtaining a careful history regarding your symptoms and your personal and family medical history, your doctor will need to perform an examination. This usually consists of careful inspection of the outside of the anus, placement of a finger through the anus into the rectum (digital examination), and placement of a finger-sized instrument through the anus to allow visual inspection of the hemorrhoidal tissue (Proctoscopy).
At times a Barium study or Colonoscopy may be advised if your doctor suspects any other cause of bleeding that needs to be ruled out.
DO PILES HAVE GRADES / TYPES?
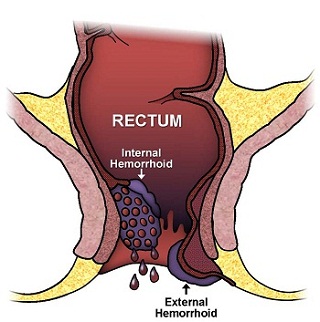
There are two main types of hemorrhoids: internal and external. Internal hemorrhoids are not sensitive to touch, pain, stretch, or temperature, while external hemorrhoids are covered by skin that is very sensitive.
When talking about hemorrhoids, one needs to understand the meaning of 'prolapse'. The anal cushions are normally fastened in the sphincter by muscles and tissue. In case too much pressure is applied, as on straining, the system of securing these cushions is damaged. Subsequently, they protrude outside the anus and this protruding mass is called the prolapse.
Internal hemorrhoids are thus graded by the degree to which they have prolapsed into:
- Grade 1 : Slightly enlarged hemorrhoidal tissue with no prolapse.
- Grade 2 : Prolapse that protrudes on pressure but goes back on its own
- Grade 3 : Prolapse that needs to be manually pushed in by the patient
- Grade 4 : Prolapse that constantly remains on the outside and does not go back even on manual repositioning. At this stage they are usually painful.
External hemorrhoids usually occur as a painful lump outside the anus. In case of clot formation ( Thrombosed external hemorrhoid ), there may be severe pain.